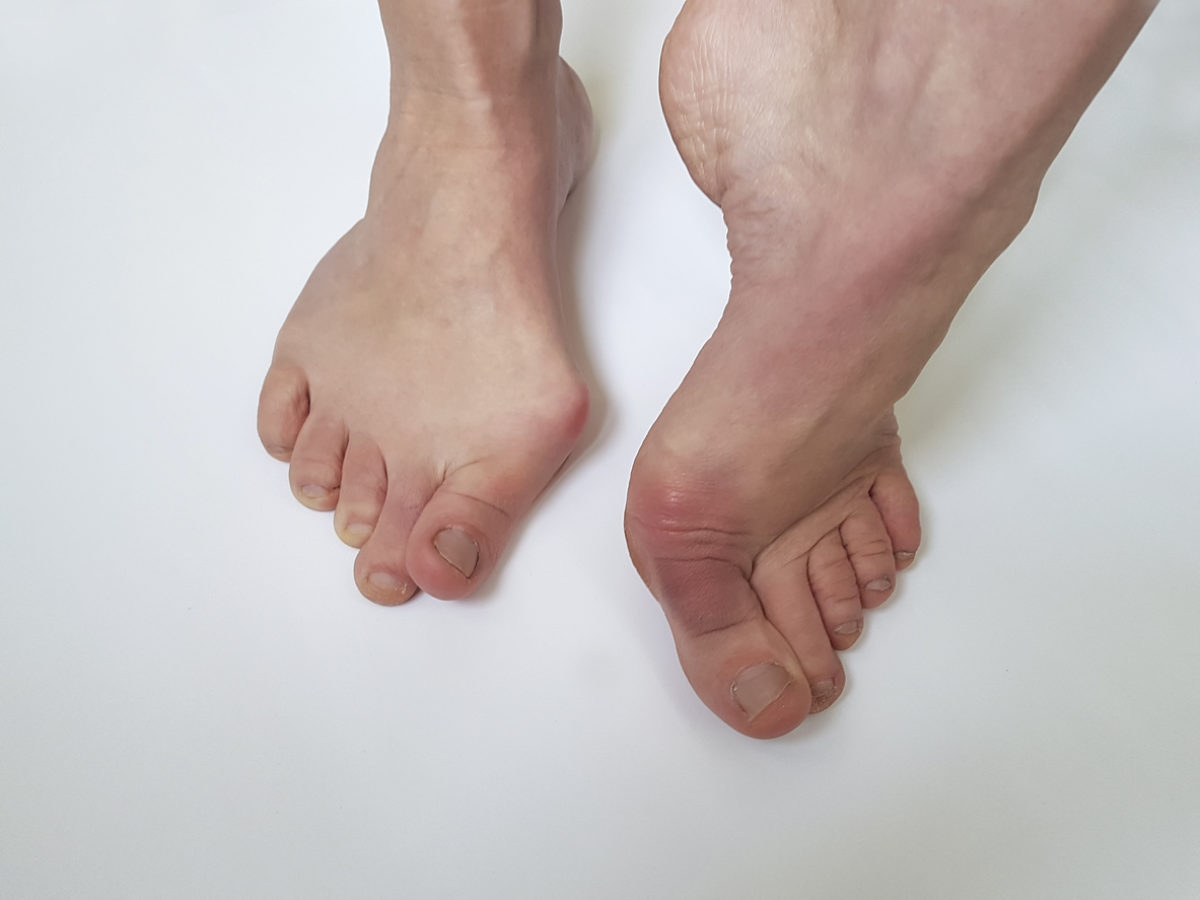
A bunion is a bony prominence on the inner aspect of the base of the big toe. Bunions are extremely common in the United Kingdom. The cause of bunions remains uncertain although they seem to be more common in families where bunions are prevalent and there is some evidence to suggest that wearing narrow shoes may also be a cause. A large number of patients with bunions do not require surgical treatment. It is only when they become painful and when conservative treatment is unsuccessful that surgery should be considered.
Bunions normally coexist with hallux valgus; a condition characterised by the big toe drifting off towards the second toe. Provided that there is no arthritis in the big toe joint, surgical treatment for bunions involves removing the bony prominence and also correcting the associated hallux valgus deformity by cutting and realigning the bone; an operation known as an osteotomy.
There are three different type of osteotomies ; the chevron, the scarf and the basal osteotomies to treat the spectrum of bunion deformities which all have good results in the scientific literature. The type of osteotomy recommended is dependent on how severe the deformity is.
These are common deformities that often present with the affected toe being painful and rubbing on shoes or the neighbouring toe. Surgical correction is indicated if conservative measures fail. The correction recommended depends on the nature of the deformity which may be of two types; flexable or fixed.
For a flexable deformity, when the toe can be easily corrected, a soft tissue procedure is recommended. The soft tissue procedure performed depends on the position of the toe but would involve either a tenotomy (tendon release), a tendon lengthening, a capsulotomy (soft tissue joint release), or tendon transfer (reattaching one tendon to another).
Plantar fasciitis is a common cause of heel pain which typically presents at the base of the heel and is worse in the morning. It is normally self limiting but may take 18 months to resolve. Conservative treatment involves pain killers, heel pads and physio. Night splints, steroid injections and ultrasoundtherapy may also be helpful. Surgical treatment involves the release of the plantar fascia, although this is rarely necessary.
There are many different types of arthritis that may affect joints; osteoarthritis and rheumatoid arthritis are the two commonest seen in the foot and ankle. Osteoarthritis refers to a degenerative loss of cartilage that normally lines the joint. It is seen as patients get older or may be a result of a previous injury that has disrupted the joint.
Rheumatoid arthritis is an inflammatory condition that causes destruction of bone and cartilage. Both conditions commonly present with pain, swelling and reduced mobility. If the pain is severe and does not respond to conservative measures, then surgery is considered. The options of surgical intervention for arthritis of the foot and ankle include:
This may be helpful in rheumatoid disease or osteoarthritis of the big toe joint but it is unlikely to provide long lasting pain relief.
Performed for the big toe where the upper part of the arthritic joint is removed.
Useful for osteochondral defects and tears in the cartilage in the ankle joint which may be curetted or shaved.
It involves the refashioning and subsequent stiffening of the joint with high levels of patient satisfaction when correctly performed.
Treatment for all fractures of the foot and ankle including calcaneal, pilon and lisfranc injuries.
Treatment for all sports injuries of the foot and ankle including chronic ankle sprains, chondral/osteochondral defects of the ankle, midfoot sprains, stress fractures, sesamoid injuries, freibergs disease and nerve entrapment syndromes.